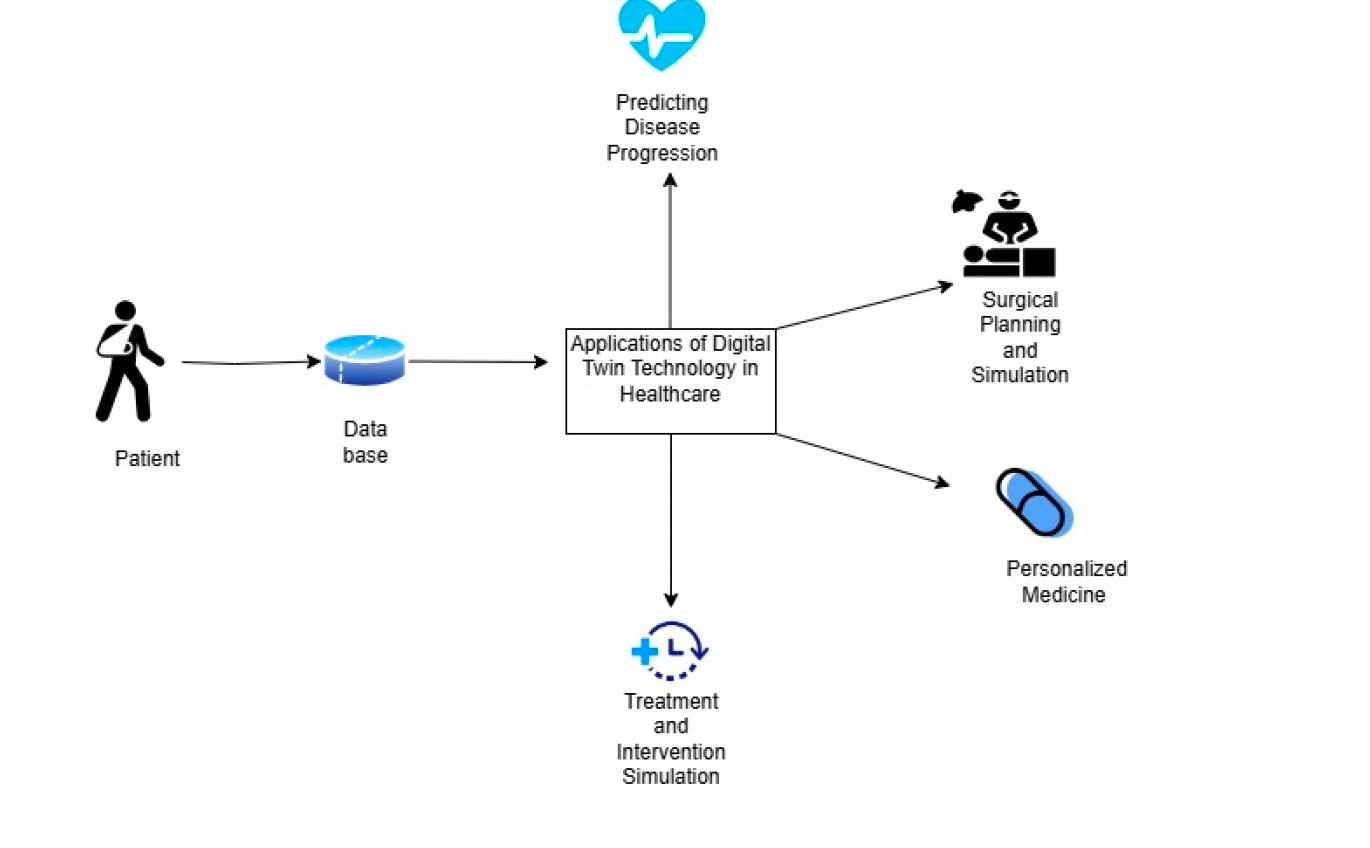
Imagine if every patient in your health system had a living digital “mirror” – a virtual version of themselves that updates in real time with their vitals, labs, and lifestyle data. This digital patient twin lets your team test treatments before trying them on the real patient, predict health issues before they happen, and personalize care like never before. It sounds futuristic, but this concept is quickly becoming a reality in healthcare. In this article, we’ll demystify what a digital patient twin is, how it’s different from the digital tools you already use (think EHRs and remote monitoring dashboards), and why healthcare leaders are paying attention now. We’ll also look at a few practical examples – from reducing readmissions to streamlining clinical trials – and close with steps for executives interested in piloting this technology.
What Is a Digital Patient Twin?
In simple terms, a digital patient twin is a virtual model of an individual patient. A computerized copy that mirrors the person’s health status and can forecast future changes. Think of it as a highly sophisticated avatar of a patient’s body and health. Unlike a static medical record, the twin is dynamic: it continuously pulls in real-time data (from wearable devices, sensors, medical imaging, etc.) and updates itself to reflect the patient’s current condition. This means the digital twin isn’t a generic/synthetic template, but a personalized digital duplicate tied to the patient’s unique health profile.
Going Beyond Traditional Digital Tools (EHRs, RPM, etc.)
How is a digital patient twin different from the digital health tools you already know, like Electronic Health Records (EHRs) or remote patient monitoring (RPM) dashboards? The easiest way to explain it is that a digital twin is not just a data repository or an alert system, it’s a livingmodel that can think ahead. A remote monitoring dashboard might show you today’s blood pressure or send an alert if a reading is out of range. These are valuable, but they are fundamentally static or reactive tools. In contrast, “a digital twin is more than a 3D model or a dashboard. It is a living, data-driven replica” that synthesizes data from many sources into actionable insights. Rather than just visualizing data, the twin continuously ingests inputs (wearable sensor readings, lab results, medical images, even social determinants) and runs analyses or simulations on that combined information Consider an RPM program for heart failure patients: the traditional approach might collect weight and blood pressure daily and alert a nurse if thresholds are exceeded. A digital twin of a heart failure patient, on the other hand, would integrate those vitals plus the patient’s medications, history, lifestyle factors, and perhaps even genomic data and then forecast deterioration before the tipping point is reached. It’s the difference between simply monitoring and truly predicting and simulating. In fact, digital twin technology “fuses together a wide range of data sources beyond the traditional medical record to forecast an individual’s future health and risks. Another key difference is the ability of a twin to allow virtual experimentation. With an EHR or dashboard, we typically react to data points. For instance, clinicians could use a patient’s twin to try out different treatment plans (virtually) to see which is likely to work best for that specific patient’s physiology before deciding on a real treatment. This is a game-changer for personalized medicine.
Why It Matters Now (in 2025)
Digital twin concepts have been around for years in industries like aerospace and manufacturing, but only now are they hitting healthcare in a meaningful way. Why 2025? There are a few converging reasons making digital patient twins especially relevant today:
● AI and Data Maturity: We finally have the AI, and cloud computing muscle to make digital twins feasible at scale. In the past, we didn’t
have the processing power or algorithms to continuously update and analyze a patient’s complex data in real time. Now, thanks to
advances in machine learning and predictive analytics, a twin can “digest” everything from vital signs to genomics and detect subtle
patterns. The growth of IoT and cloud means we can stream and crunch vast amounts of health data quickly.
● Wearables and Remote Monitoring Ubiquity: The past few years have seen wearable health devices go mainstream. Approximately
35% of U.S. adults now use a wearable health device (like a smartwatch or fitness tracker), and 40% use health-related apps. Globally,
the wearables market is booming, meaning millions of people are continuously collecting heart rates, oxygen levels, glucose readings,
and more. This ubiquity of real-time patient data is fuel for digital twins. It’s hard to build a live updating twin if you only have an annual
check-up’s worth of data. But if a patient is streaming data 24/7 from their wrist, scale, or implantable device, the twin becomes a rich,
constantly refreshed model. By 2026, health systems are awash in data from connected devices – the opportunity (and challenge) is to
turn that raw data into meaningful predictions. Digital twins are one answer: they take all those data points and integrate them into a
coherent, usable narrative of the patient’s health trajectory.
Use Cases Driving ROI and Better Outcomes
It all sounds promising in theory, but what can a digital patient twin actually do for a health organization? Here are a few high-impact use cases in 2026 that show real operational value:
1. Streamlining Clinical Trials and Improving Inclusion: Pharma companies and academic medical centers are exploring “virtual
clinical trials” using digital patient twins to speed up research and make trials more inclusive. In traditional trials, recruiting patients (and
making sure the trial group represents diverse populations) is a huge challenge. With digital twins, researchers can simulate aspects of
a trial in silico. For example, AI-driven disease models can generate a “virtual control group” of patient twins, allowing real patients to all
receive the experimental treatment (fewer on placebo) and still have solid comparative data.
2. Digital twins also help design better trials upfront: before starting a study, investigators can run simulated trials on twin populations to
refine their inclusion criteria and endpoints for higher success rates. In terms of inclusion and diversity, imagine being able to test how a
proposed trial would perform if more patients of a certain demographic or co-morbidity profile were included – the twin simulations might
reveal unanticipated risks or needed adjustments, thereby guiding researchers to design trials that safely include those groups. All of
this means potentially faster drug development, lower costs, and trials that more closely reflect real-world patient populations. For
healthcare providers involved in research or just awaiting new therapies, that’s a big win. It’s a great example of how digital twin tech
isn’t just operational hype; it’s tangibly improving processes in healthcare R&D.
How Infiuss Health puts digital twins to work
What we do
Infiuss Health provides a Digital Patient Twin platform that lets care and research teams rehearse decisions before they touch real patients. We build high-fidelity patient models from de-identified EHRs, multi-omic data, and continuous wearable streams, then run protocol and workflow simulations to forecast outcomes, costs, and risks. Our platform integrates with your existing stack, including our PROBE CTMS or third-party systems like Medidata and Veeva, so results flow into day-to-day operations.
Where it helps first
Trial design and research operations
● Simulate inclusion and exclusion criteria, dosing schedules, and visit plans to predict enrollment, drop-off, adverse events, and total
study timelines.
● Map where eligible patients actually are to guide site selection and reduce screen fails.
Use virtual control arms and risk-based follow up to shrink control cohorts and cut avoidable visits while maintaining statistical power.
● Monitor for protocol deviation and get corrective and preventive action suggestions before issues snowball.
Infiuss Health.pptx (3)
Clinical decision support (in progress)
● Individual patient twins support forecasting of adverse events and dose adjustments, starting with high-impact therapeutic areas where
continuous data are available.
Early programs have shown meaningful operational wins: fewer protocol amendments, smaller required cohorts for the same endpoints, and
months shaved off study timelines, which translate into material cost avoidance and faster evidence generation for care pathway decisions. For
example, partners have seen reductions in enrolled patients versus the initial protocol design and 6 or more months saved per study.
Ready to explore the possibilities? Consider reaching out to innovation partners or internal champions to kickstart a digital twin pilot, and see
first-hand why so many in the industry believe this is the next big leap for healthcare. The future where every patient has a digital twin is coming
and it’s one where executives who champion such innovations will find their organizations at the forefront of quality and efficiency in care.